COMMUNITY DIGEST
Five featured cases, two quick consultations, and a handful of shared references from the EndoCollab WhatsApp community between March 21 and April 10, 2026. An inverted appendix appendicitis on colonoscopy. A steroid-refractory checkpoint colitis in a complex host. Chicken skin mucosa at the base of a villous adenoma. A two-decade autoimmune hepatitis patient on cyclosporine. And a high-density recap of severe alcoholic hepatitis management in 2026.
Compiled by EndoCollab · Cases and teaching points curated from the EndoCollab private WhatsApp community.
In this issue
- Inverted Appendix Appendicitis on Colonoscopy
- Steroid-Refractory Checkpoint Colitis: Escalating to Infliximab in a Complex Host
- Chicken Skin Mucosa and the Adenoma It Marks
- Autoimmune Hepatitis on Cyclosporine for Two Decades: Switch, Stop, or Rebiopsy?
- Alcoholic Hepatitis in 2026: What Still Works, What Doesn’t
- Quick cases: Coca-Cola for fecaloma; hold GLP-1 and GIP before OGD
- Community notes: surgical stump inversion, ACG AH guideline, LAMS complication review, mesenteric vein thrombosis
Featured Cases
1. Inverted Appendix Appendicitis on Colonoscopy
A colonoscopy series was shared with the caption “inverted appendix appendicitis.” The appearance was striking enough that the group took it in several directions before converging on a recommendation.
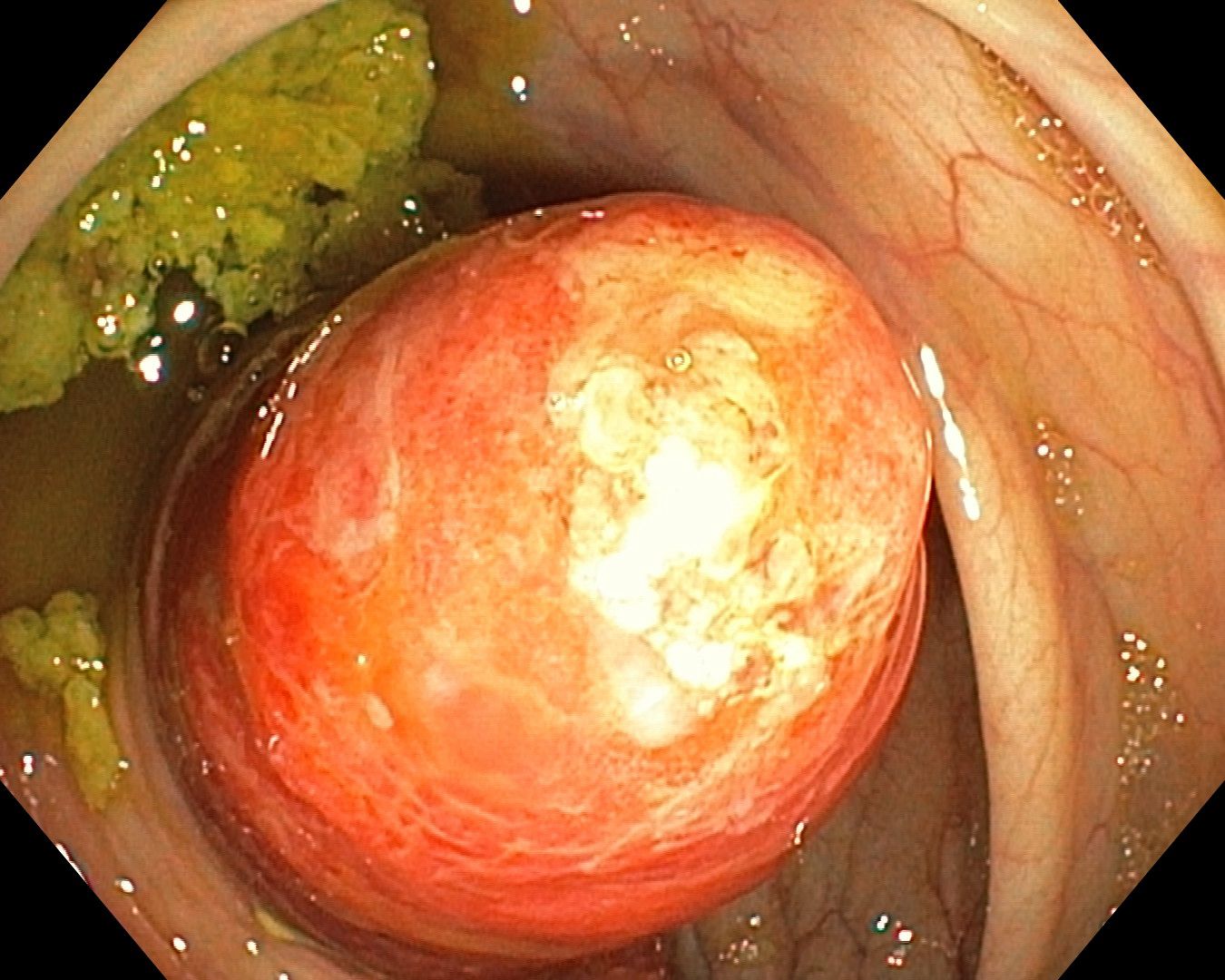
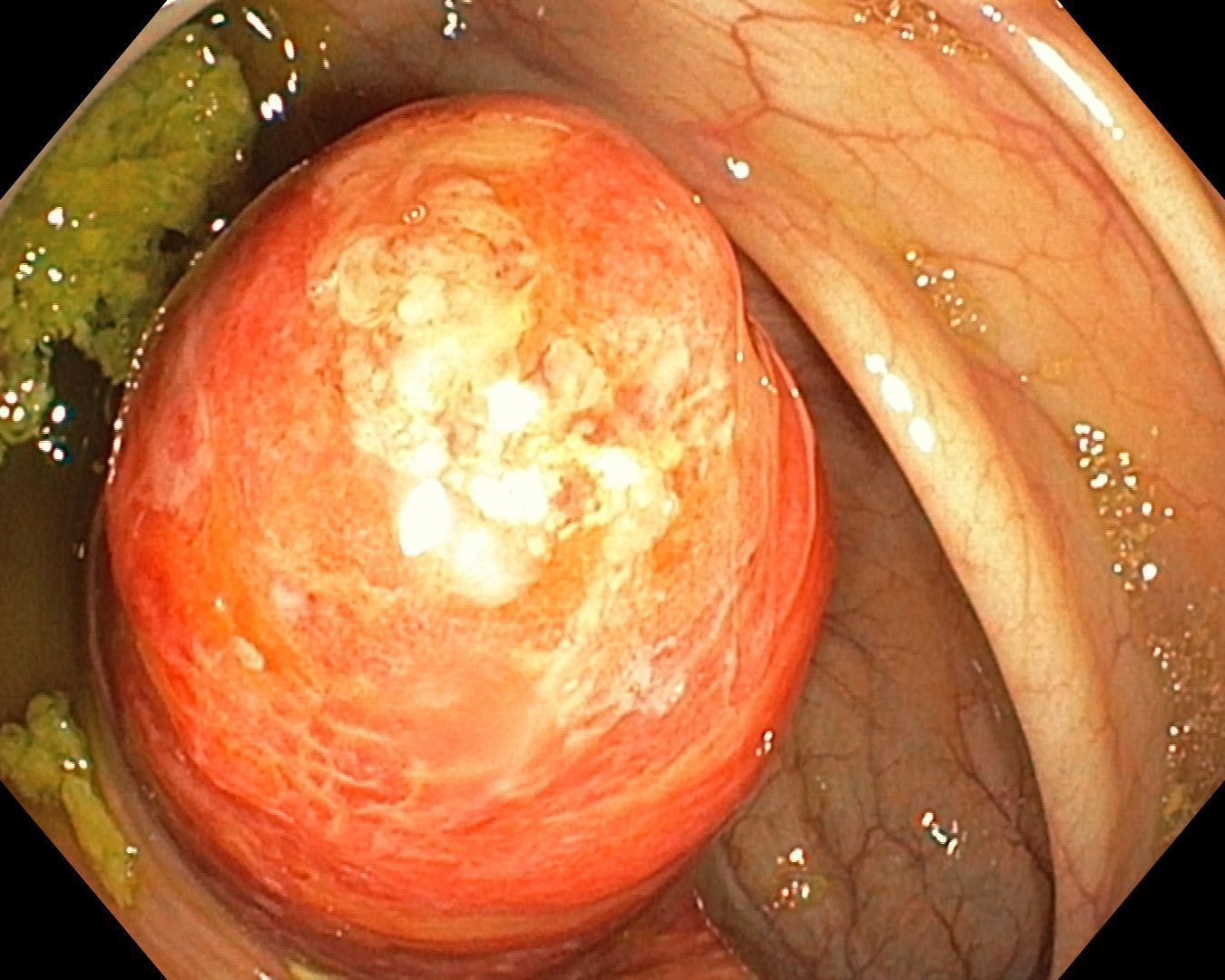
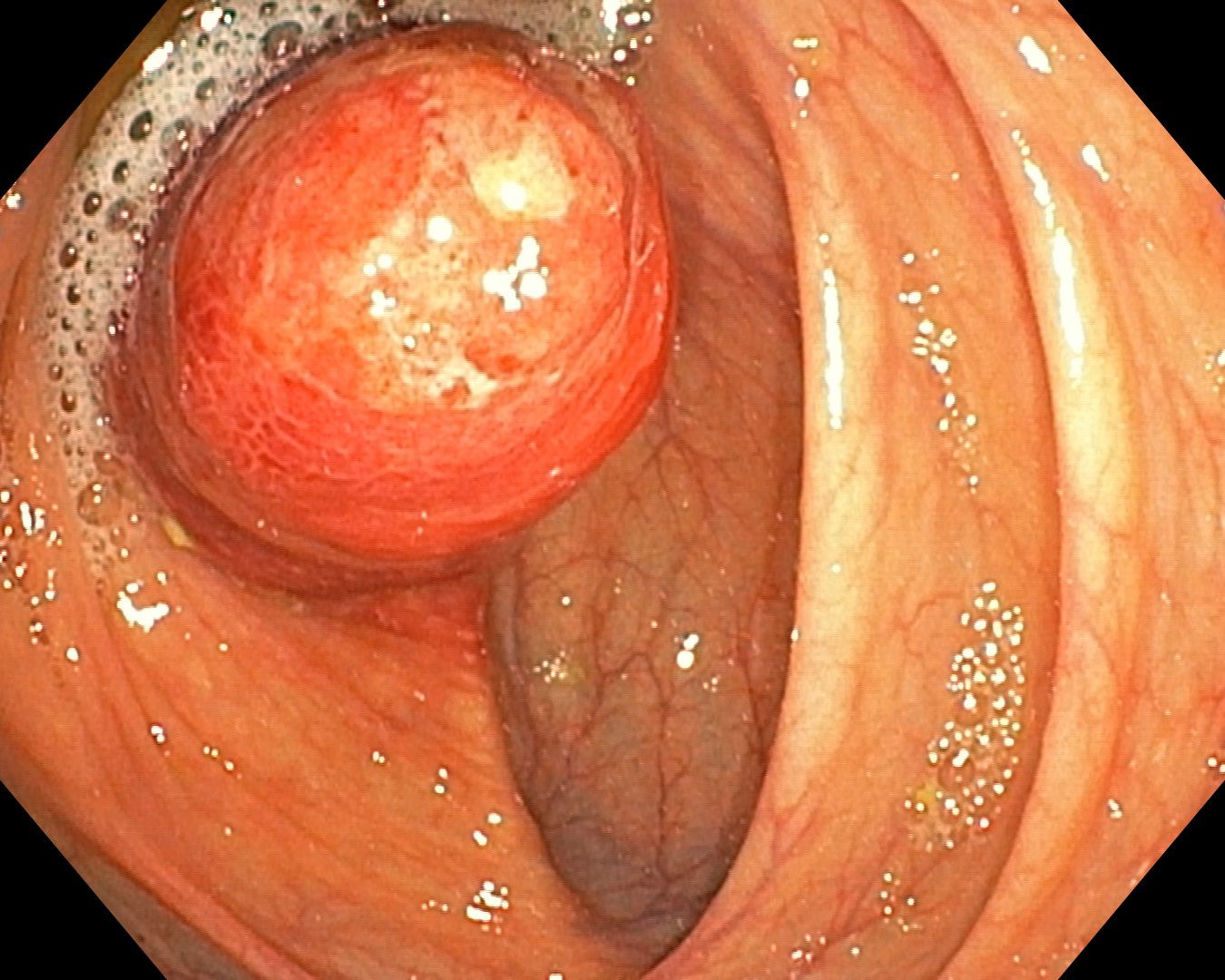
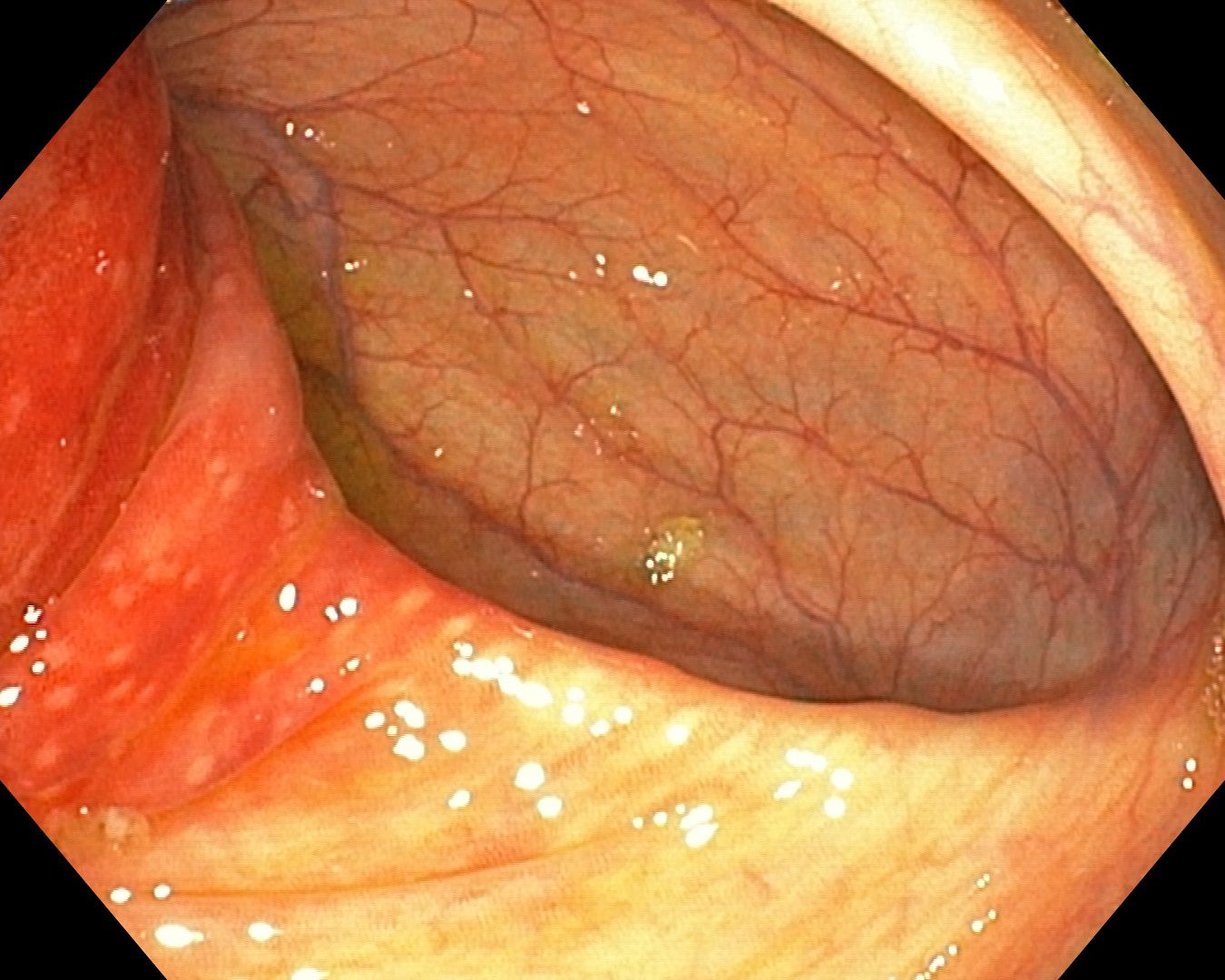
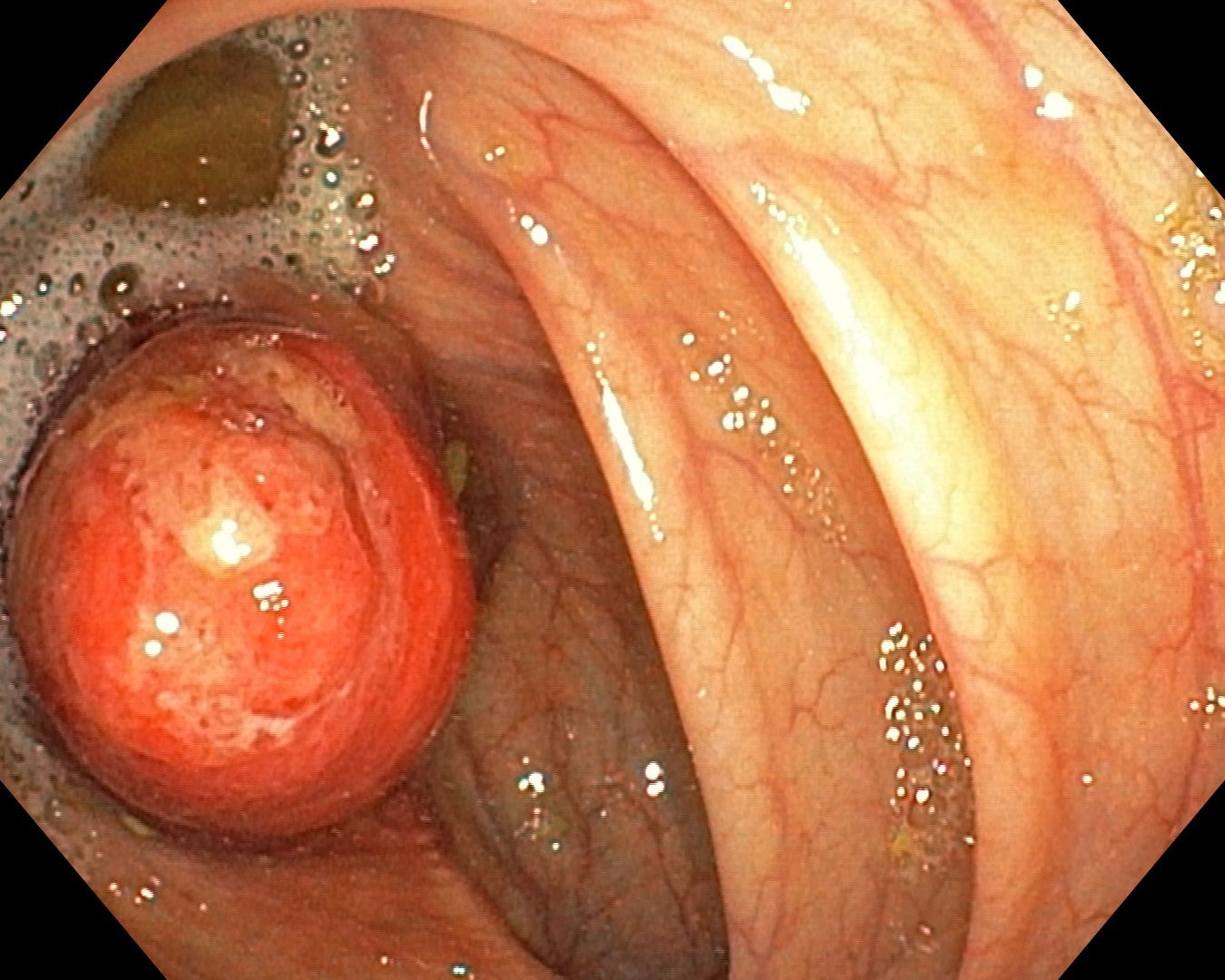
The first question raised was history. Had the patient had a prior appendectomy? In older open surgical practice, general surgeons routinely buried the appendiceal stump with a purse-string suture. That buried stump can project into the cecal lumen and mimic an inverted appendix decades later. Mucocele and appendiceal adenoma were also offered as real differentials that shouldn’t be dropped just because the cecum “looks inverted.”
The teaching lead framed the mechanism. Conventional appendicitis follows obstruction, then infection, inflammation, distension, ischemia, and eventually perforation. Inverted appendicitis is closer to an intussusception, the pathophysiology is different, and so is the endoscopic appearance.
The group reviewed the antibiotics-only literature for uncomplicated appendicitis. Roughly one-third of antibiotic-treated patients need surgery within a year, per the Cochrane-style reviews. ERAT (endoscopic retrograde appendicitis therapy) was introduced as an evolving modality. One member noted that endoscopic appendectomy via NOTES has been performed in select centers, including at AIG Hyderabad.
Teaching point. Inverted appendicitis is mechanistically distinct from conventional appendicitis, more akin to intussusception than obstruction. The endoscopic appearance overlaps with mucocele, appendiceal adenoma, and old purse-string stump inversion, so context and imaging still matter. Laparoscopic appendectomy remains the standard; ERAT and endoscopic appendectomy via NOTES are emerging options with limited reach.
2. Steroid-Refractory Checkpoint Colitis: Escalating to Infliximab in a Complex Host
A 68-year-old man with lung cancer on Keytruda developed checkpoint colitis in January. He improved on steroids. Keytruda was stopped. He then developed adrenal insufficiency and was maintained on prednisone 5 mg daily. A month later he returned with chronic abdominal pain and diarrhea. EGD showed severe duodenitis and candida esophagitis. Flex sig of the distal colon looked OK. CMV PCR, C. diff, and stool culture were all negative.
Working diagnosis was checkpoint enteritis. Three days of IV solumedrol did not produce a response. The patient was sick, mottled legs and abdomen, severe abdominal pain. The team was considering infliximab, but the concurrent candida esophagitis made escalation uncomfortable.
The teaching lead reframed the case around adrenal physiology. Adrenal insufficiency in this patient could come from bilateral adrenal metastases or autoimmune adrenalitis from Keytruda. Keytruda had been stopped and prednisone 5 mg had been enough for a while, but the current picture may represent progression, worsening adrenal insufficiency from metastases, which could explain the lack of response to solumedrol. Mineralocorticoid replacement might be needed.
Another member agreed that infliximab was a reasonable next step, with vedolizumab as an alternative, but flagged the usual surrounding workup: pancreatic enzymes, CT abdomen to rule out perforation, sepsis workup, and broad-spectrum antibiotics. The presenter replied that AM cortisol was high and BP was normal on admission, arguing against pure adrenal failure. Repeat CT abdomen showed enteritis only, no perforation. The patient was already on antibiotics.
Teaching point. Steroid-refractory immune-checkpoint-inhibitor colitis and enteritis are established indications for infliximab or vedolizumab. But parallel reasoning still matters: opportunistic infection, pancreatic involvement, perforation, and underlying adrenal physiology can all masquerade as, or coexist with, a failed steroid response. Candida esophagitis is a relative concern with IFX but not a hard contraindication in a sick checkpoint-enteritis patient.
3. Chicken Skin Mucosa and the Adenoma It Marks
A colonoscopy image was posted with the question: “Does this look like NG-LST?” A pedunculated-appearing polyp sat on a base that extended laterally across two folds. Arrows highlighted the extension.
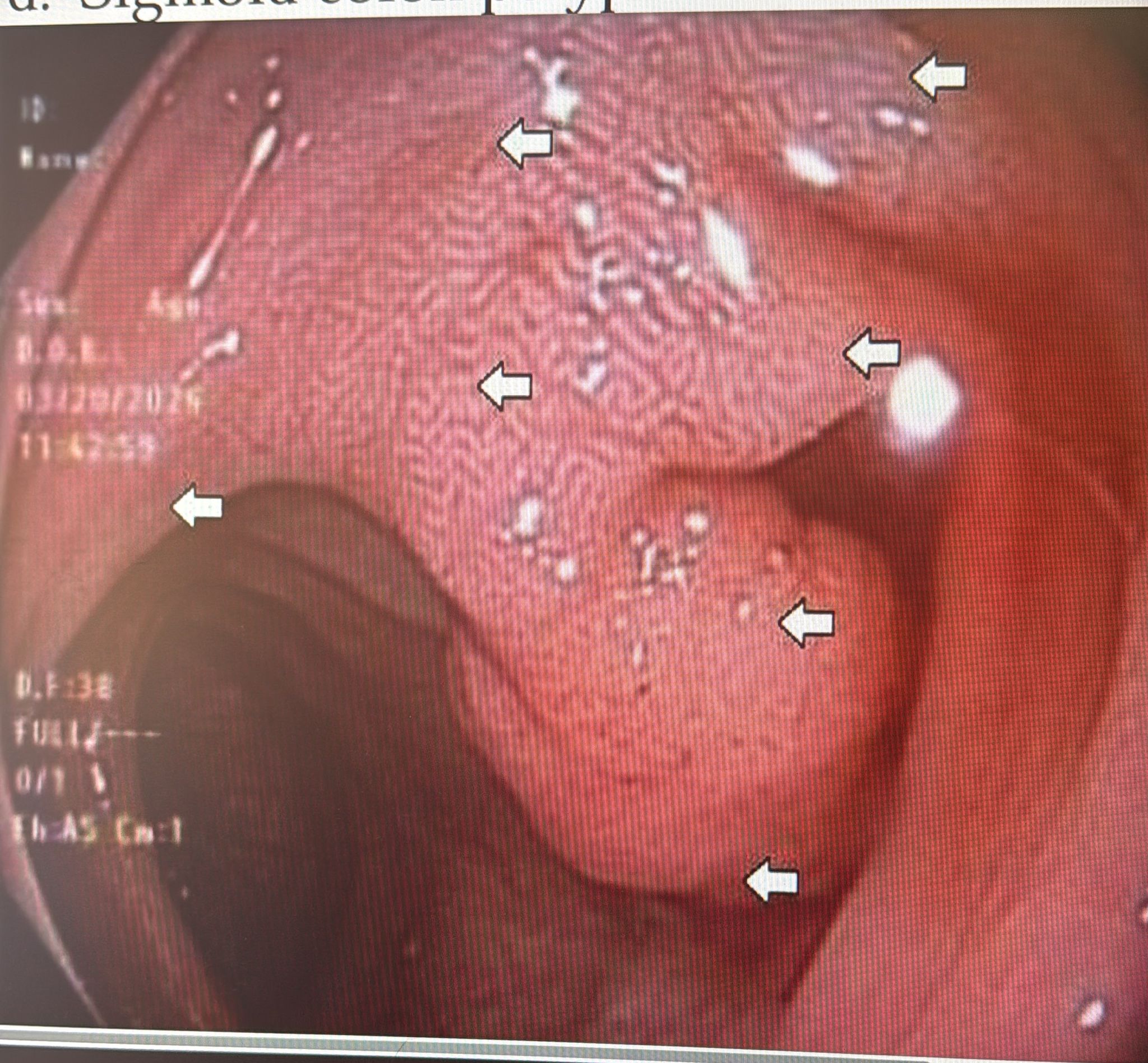
One member read it as a pedunculated polyp with a small stalk. The presenter agreed the overall shape looked pedunculated but argued the base itself was adenomatous. Other members called out the “chicken skin” (Hakuhan) appearance at the base and interpreted it as supportive of adenoma, not a separate lesion. Biopsy returned villous adenoma, matching the macroscopic read.

The teaching lead framed it clearly. Chicken skin mucosa points to a higher grade of dysplasia within an adenoma and a greater risk of submucosal invasive carcinoma. The villous histology is proof of the concept. Pit pattern, vascular pattern, and polyp size all still have to feed into the resection decision.
The practical question came next: should we cut out the “chicken skin” when doing the polypectomy? The answer was no, but its presence should influence the choice between simple cold-snare polypectomy and EMR or ESD once optical diagnostics (NICE, JNET, Kudo) and size have been factored in.
Teaching point. Chicken skin mucosa (Hakuhan) at the base of an adenomatous polyp is a visual flag for higher-grade dysplasia and elevated submucosal invasion risk. It does not need to be resected as a separate lesion, but seeing it should push your resection strategy toward a more definitive technique (EMR or ESD) rather than simple cold-snare polypectomy when size and optical diagnosis allow.
4. Autoimmune Hepatitis on Cyclosporine for Two Decades: Switch, Stop, or Rebiopsy?
A patient in her 70s had been on cyclosporine for autoimmune hepatitis since 2007, nearly two decades. She had just been admitted for a new prescription and remained in biochemical remission. Cyclosporine is not first-line for AIH, carries a meaningful side-effect burden, and the original decision-making from 2007 was not available. The presenting physician’s question: how do you move a long-remission patient off cyclosporine onto more conventional therapy?
One member asked why switch at all. AIH patients on cyclosporine are uncommon in his experience. He noted that MMF has become more popular as first-line since the Camaro trial. Another member confirmed tacrolimus yes, cyclosporine not typical.
The teaching lead pushed the work-up back to first principles. How long has the patient been on cyclosporine? What are the current transaminases and IgG? Which antibodies were positive at diagnosis? How long has she been in biochemical remission? What did the initial liver biopsy show? All of those have to feed the decision to switch, taper, or stop. A rebiopsy was suggested: if histology looks clean after two decades of biochemical remission, consideration of treatment withdrawal is reasonable.
The presenter did not have access to the 2007 biopsy or labs. The teaching lead initially wondered whether this was a young patient started in childhood, cyclosporine is sometimes chosen over steroids to avoid growth suppression in pediatric AIH. The presenter clarified that the patient is around 70, which refocused the decision from “switch immunosuppressants” toward “rebiopsy and reassess the case for withdrawal.”
Teaching point. In autoimmune hepatitis, cyclosporine is not first-line, and the modern preference is MMF or, less commonly, tacrolimus. A patient in multi-year biochemical remission on an older agent is a candidate for a diagnostic rebiopsy and a considered trial of treatment withdrawal, not automatically a lateral switch to another calcineurin inhibitor. Restart the case from baseline labs, antibody profile, and histology before assuming the plan is “swap drugs.”
5. Alcoholic Hepatitis in 2026: What Still Works, What Doesn’t
A quick aside inside a longer thread turned into a high-density teaching recap. “Do you guys do steroids for severe alcoholic hepatitis or not bother?”

The teaching lead laid out the current standard. Maddrey DF greater than 32, with or without hepatic encephalopathy, gets prednisolone 40 mg daily. The Lille score at one week guides continuation or stop. Do not use steroids with sepsis, acute renal failure, or active GI bleeding. If steroids are contraindicated, pentoxifylline used to enter the conversation.
Another member corrected that last point. Pentoxifylline is no longer indicated, no current trial support. For ALF and acute-on-chronic liver failure presentations, plasmapheresis is an option. The teaching lead thanked him for the update, noting he had not managed AH since 2016; his reference point was the older Akriviadis trial, which showed a short-term mortality benefit, and STOPAH, which refuted that benefit.
A third member added practical experience. Pentoxifylline had no role in his recent cases. Plasmapheresis brings bilirubin down well. He tried G-CSF in one patient who improved. Treatment options for AH-ACLF are genuinely limited. On hepatorenal syndrome, terlipressin plus albumin works well as a bridge.
The framing everyone returned to: DF greater than 32 is the difficult population; DF less than 32 does much better; abstinence is the bottom line; transplant is the destination when the DF is high and response is poor.
Teaching point. For severe alcoholic hepatitis with Maddrey DF greater than 32 and no sepsis, acute renal failure, or active GI bleed, prednisolone 40 mg daily with a Lille-score check at one week remains the standard. Pentoxifylline is out. For AH progressing to ACLF, plasmapheresis is the current most-promising salvage. For hepatorenal syndrome, terlipressin plus albumin is the bridge. Abstinence is still the biggest long-term lever, and transplant is the destination when the DF is high and response is poor.
Quick Cases
March 22 · Coca-Cola for Fecaloma and Gastric Bezoars
- Delivery is endoscopic, instillation and injection through the colonoscope.
- One case used roughly one liter of Coca-Cola instilled.
- A cheap, accessible intervention that sits alongside rectal enemas and oral laxatives in the escalation ladder for refractory fecaloma.
April 10 · Hold GLP-1 and GIP Agonists Before OGD
- Delayed gastric emptying on semaglutide, tirzepatide, and related agents is a real aspiration-risk issue.
- Pre-OGD checklist item for any patient on these agents.
Community Notes
- Old open-era stump inversion is not pediatric-only. General surgeons routinely buried the appendiceal stump with a purse-string suture before laparoscopic technique took over. That’s why an “inverted appendix” appearance can sometimes be iatrogenic rather than primary.
- Mesenteric vein thrombosis belongs in the differential for mesenteric ischemia, especially in patients with an underlying prothrombotic state and local inflammation such as diverticulitis.
What’s Next
Every case in this digest came from real conversations in the EndoCollab private WhatsApp community, 650+ practicing endoscopists discussing cases daily from every continent. Lifetime members get permanent access to the group, plus the full EndoCollab case library of 1,700+ teaching cases, technique videos, and references.


