COMMUNITY DIGEST
Five featured cases, two quick consultations, and key clinical pearls from the EndoCollab WhatsApp community between April 11 and April 25, 2026. A fatal case of hemosuccus pancreaticus with a sentinel bleed. Acute esophageal necrosis managed conservatively. A seafood allergy gastritis that turned out to be gastric neoplasm. An acute hepatitis puzzle. And UC treatment without biologics.
Compiled by EndoCollab · Cases and teaching points curated from the EndoCollab private WhatsApp community.
In this issue
- Hemosuccus Pancreaticus: The Sentinel Bleed
- Acute Esophageal Necrosis (“Black Esophagus”): When Less is More
- Post-Seafood Allergy Gastritis: From Eosinophilic Suspicion to Gastric Neoplasm
- Acute Hepatitis in a Young Male: A Diagnostic Puzzle
- UC with 5-ASA Skin Allergy: Navigating Non-Biologic Options
- Quick cases: Formaldehyde for bleeding radiation proctitis; colonic lymphoid aggregates
Featured Cases
1. Hemosuccus Pancreaticus: The Sentinel Bleed
A patient with acute on chronic calcific pancreatitis and a dilated main pancreatic duct presented with obscure UGI bleeding (melena and a small-volume hematemesis of 10-15mL). OGD and CT Angiography were both negative. The patient improved and was transferred out of the ICU.
Days later, he suffered a catastrophic 1000mL hematemesis with hemodynamic collapse. Repeat OGD showed a large clot on the D2 medial wall near the ampulla, with fresh blood extending to D3. The patient did not survive.
Dr. Madhavan had warned early: “This might be a sentinel bleed and can be followed by catastrophic bleeding.” The group recommended DSA with provocative maneuvers (intra-arterial vasodilators or heparin) as the gold standard to unmask quiescent pseudoaneurysms. EUS was highlighted as an alternative.
Clinical Pearl: A negative CTA does not rule out hemosuccus pancreaticus. Small (<3mm) or thrombosed pseudoaneurysms may be invisible on CTA. DSA is the gold standard, not a last resort.
2. Acute Esophageal Necrosis (“Black Esophagus”): When Less is More
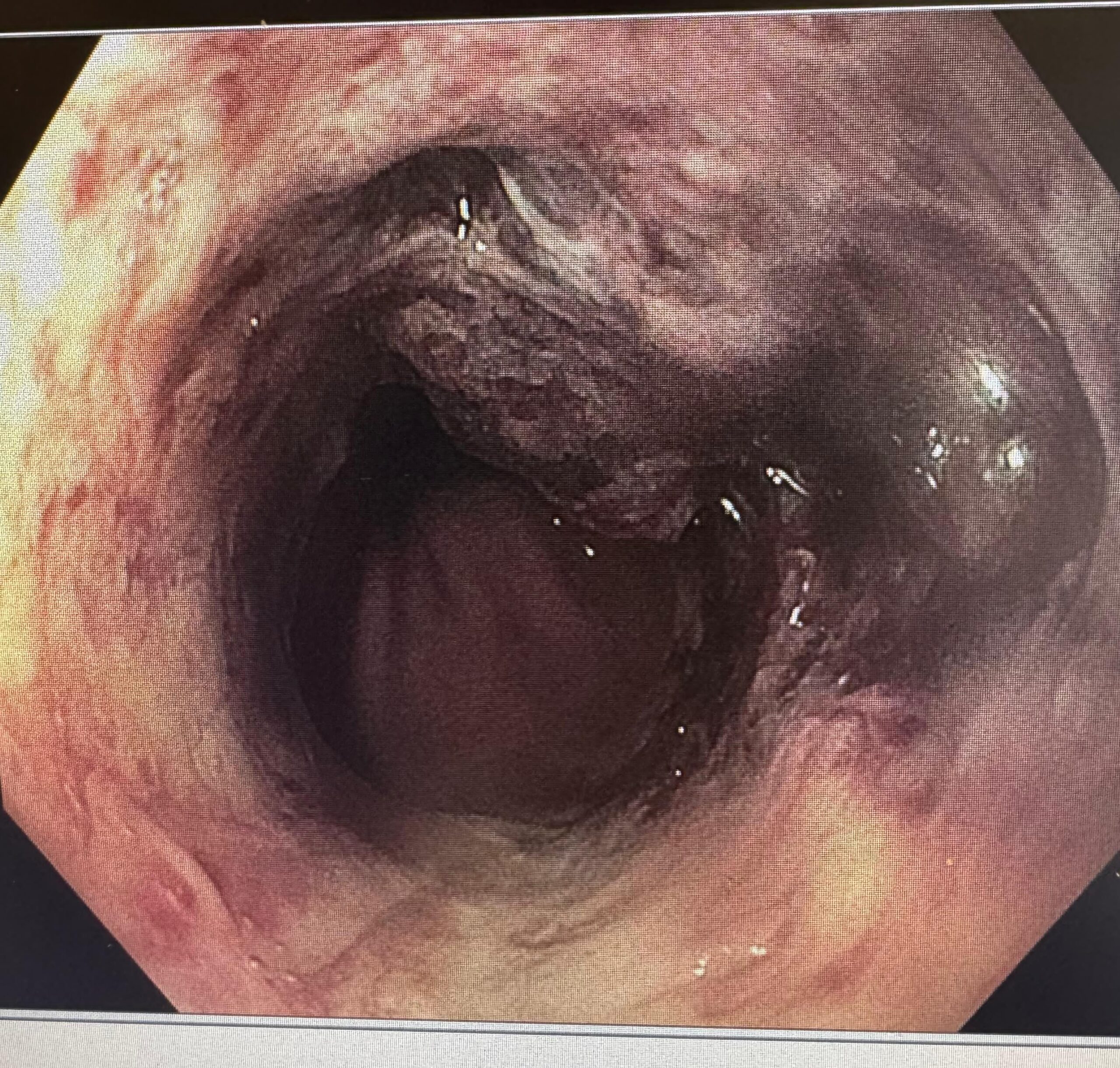
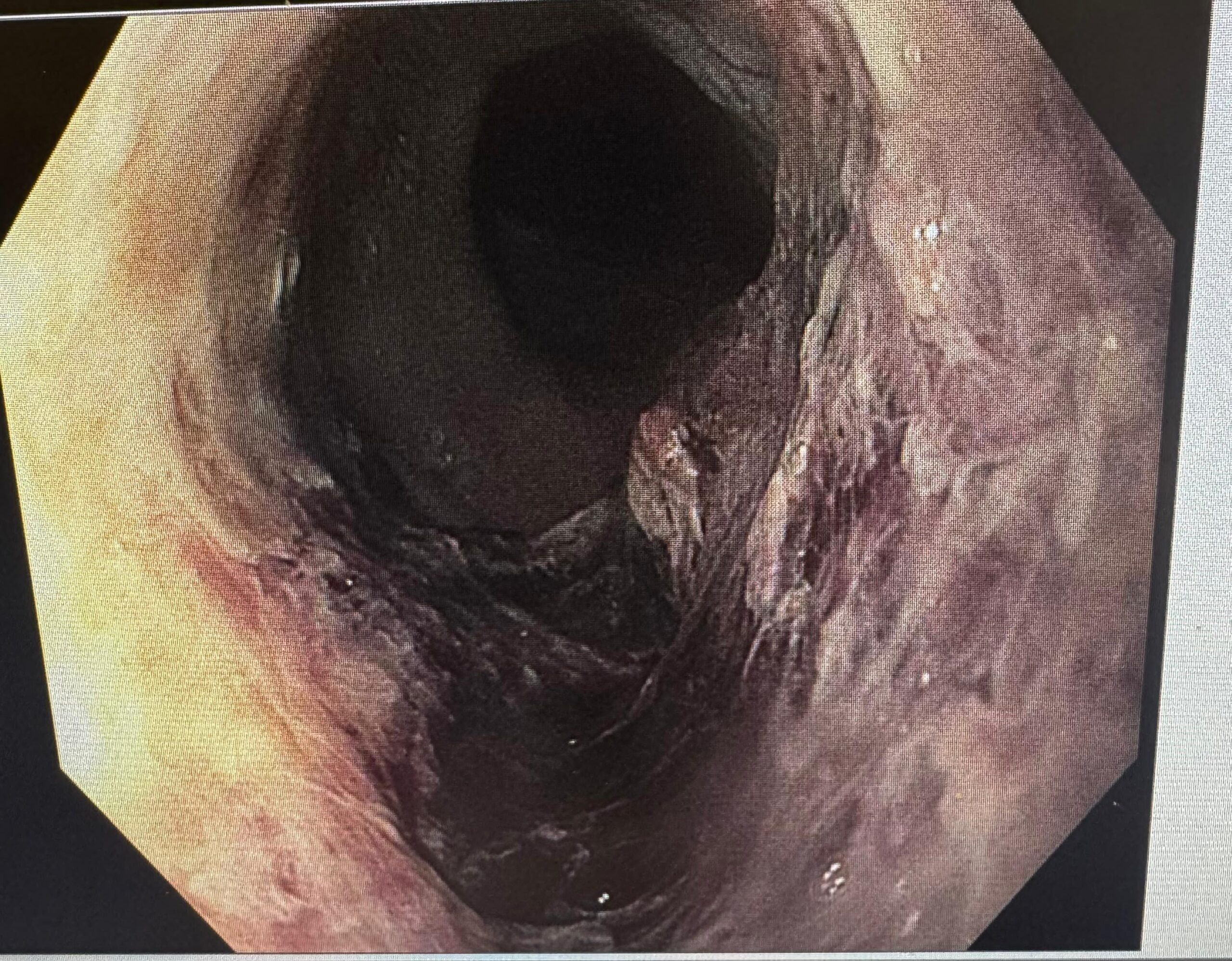
A frail 70-year-old, poor surgical candidate, presented with severe esophagitis with a very large ulcer and overlying clot. Hemospray was applied.
Dr. Alawamy identified this as “black esophagus” and outlined management: high-dose PPI, NPO, IV hydration, and TPN if prolonged. “Most times this resolves with supportive care… it may take a week or two.”
Do NOT stent: “These stents will expand and apply radial forces on the lumen, any weak points will give and cause perforation.” No NGT, no PEG. If you must re-scope, use CO2, a slim/pediatric scope, and minimize procedural time.
Useful reference: Acute Esophageal Necrosis Management Flowchart (PMC)
3. Post-Seafood Allergy Gastritis: From Eosinophilic Suspicion to Gastric Neoplasm
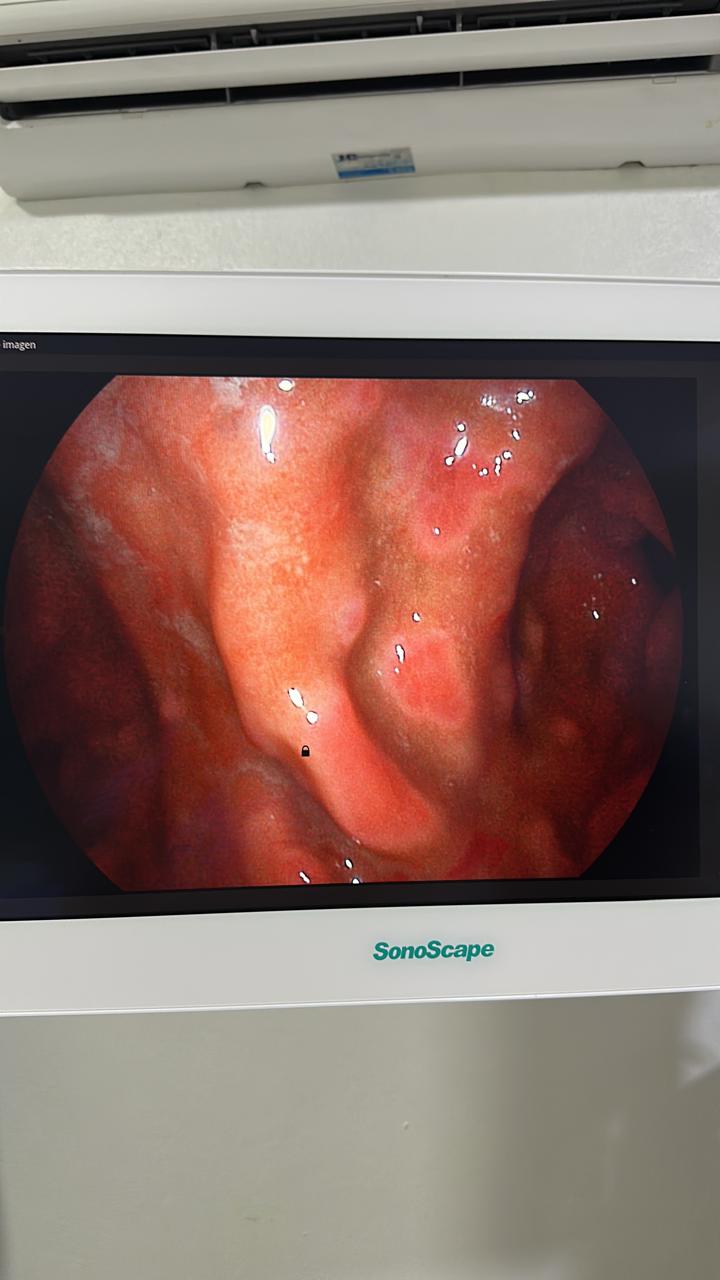
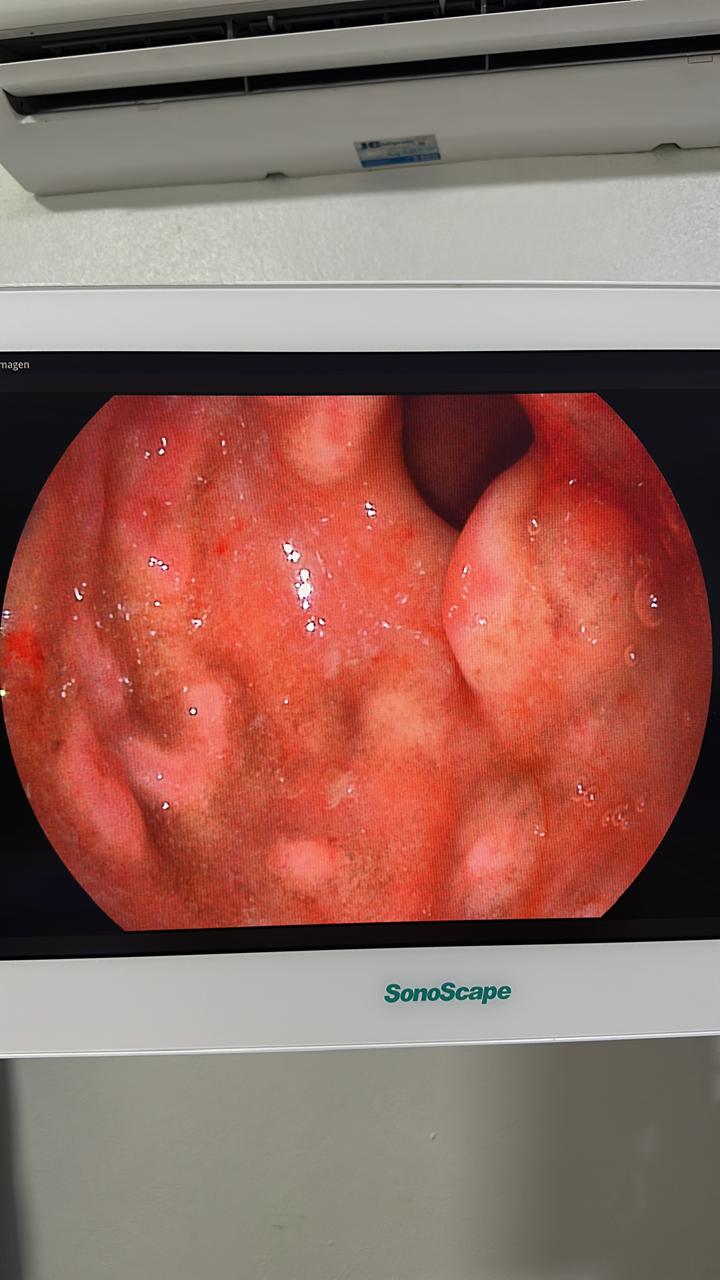
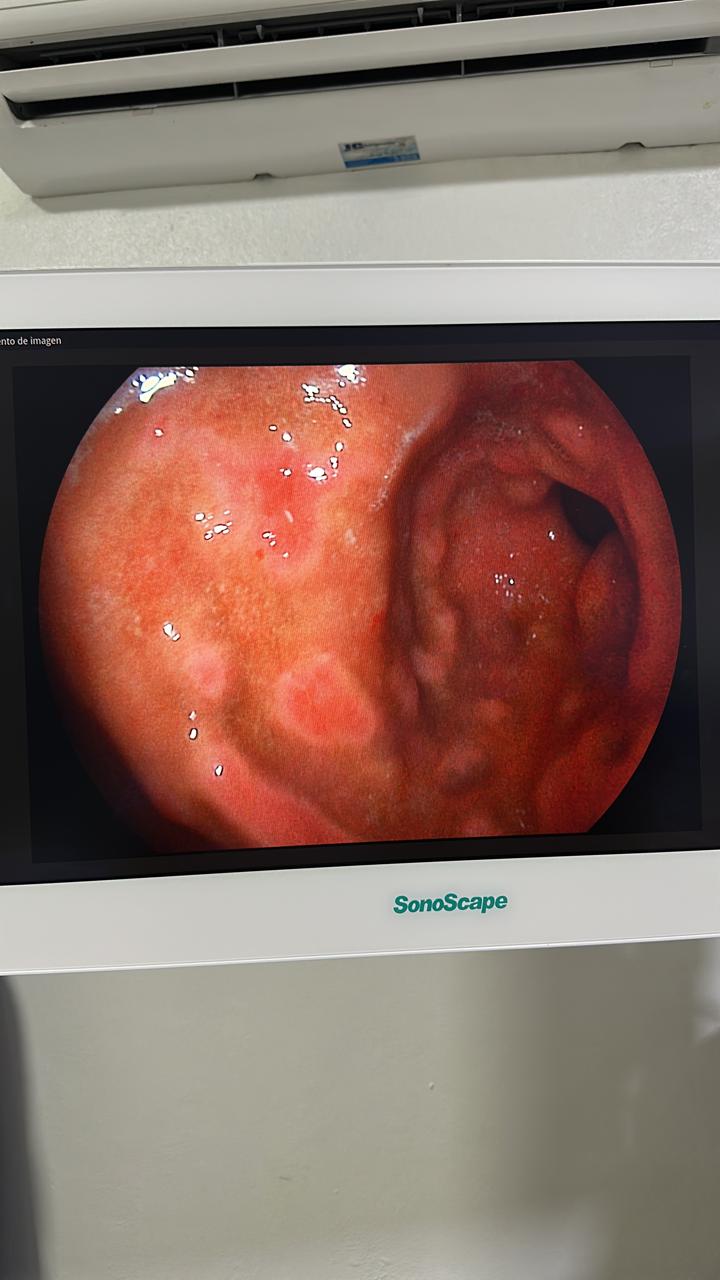
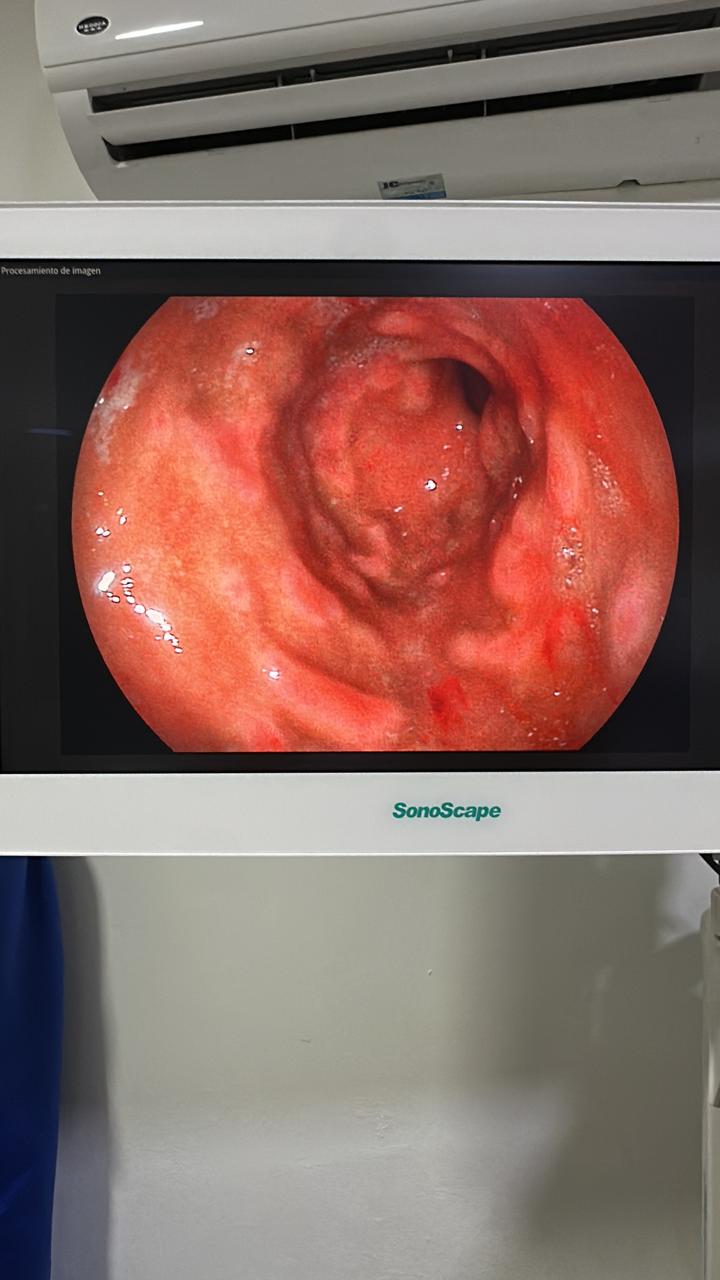
A 31-year-old female with no past medical history presented with epigastric pain, nausea, and postprandial vomiting after her first-ever allergic reaction (laryngeal edema from shrimp). EGD showed dramatic patchy erythema, edema, loss of epithelium, and nodules.
Initial DDx favored eosinophilic gastroenteritis. Dr. Klaus also flagged anisakiasis, strongyloidiasis, vasculitis, and lymphoma. Dr. Alawamy noted “the history is more important than the endoscopic findings” and recommended checking serum IgE levels.
Plot twist: Two weeks later, biopsy returned as a poorly differentiated neoplasm with features suggestive of diffuse-type adenocarcinoma vs. MALT lymphoma. IHC and molecular studies were recommended. What looked like food allergy-related gastritis turned out to be a gastric neoplasm requiring entirely different management.
4. Acute Hepatitis in a Young Male: A Diagnostic Puzzle
A young male presented with RUQ pain, fever, nausea, and vomiting. AST peaked at 1900, ALT at 500, then normalized within days. The entire hepatitis and autoimmune panel was negative. No gallstones on US.
Dr. Alawamy’s key observation: “AST was almost 4 times the ALT. Whether this is truly hepatic or non-hepatic in origin” must be questioned. He emphasized that “US is not enough to conclusively say that the CBD had a stone in it or not.”
Dr. Klaus added DILI, mononucleosis, right-sided heart failure (given the patient’s emphysema), PE, and Budd-Chiari to the differential. CK was never checked. The consensus: most likely a passed CBD stone.
Clinical Pearl: When AST far exceeds ALT, think beyond the liver. US alone cannot exclude choledocholithiasis. Always check CK to rule out rhabdomyolysis. Rapid normalization with RUQ pain points strongly toward a passed stone.
5. UC with 5-ASA Skin Allergy: Navigating Non-Biologic Options
A 40-year-old female with mild UC (70cm extent) responded well to mesalazine but developed a skin allergy. Biologics were too expensive.
Non-biologic alternatives discussed:
- Budesonide MMX (Cortiment) 9mg for 8 weeks. Use the multi-matrix formulation, NOT the immediate-release version.
- Check TPMT and start azathioprine concomitantly.
- Etrasimod (S1P modulator) is an emerging option for mild-moderate disease.
- In some regions, biosimilar anti-TNF agents are significantly cheaper.
Quick Consultations
Formaldehyde for Bleeding Radiation Proctitis
Formalin application is effective, especially when APC is difficult at the linea dentata. Despite promising data, handling safety concerns remain a barrier to wider adoption.
Colonic Lymphoid Aggregates
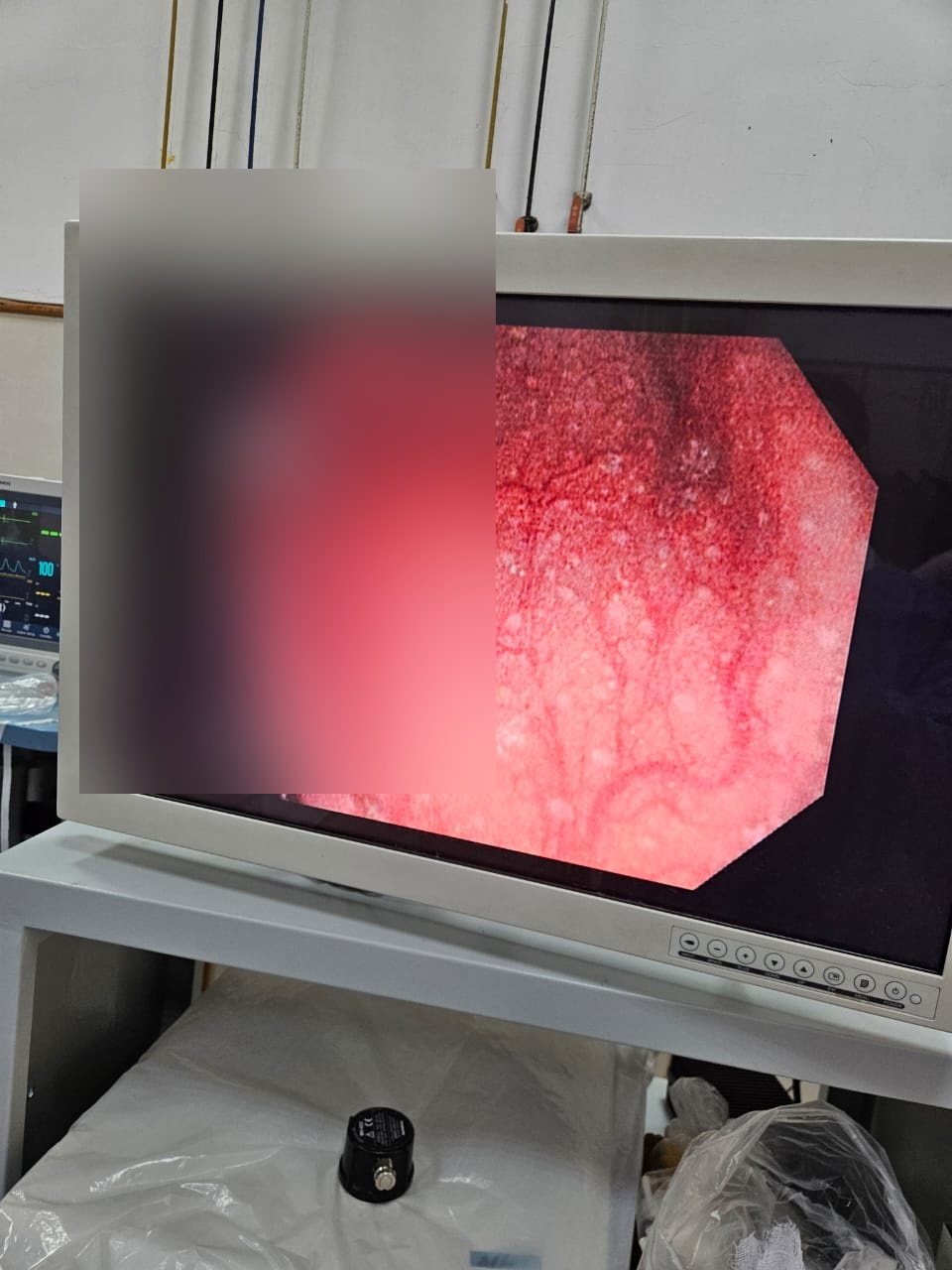
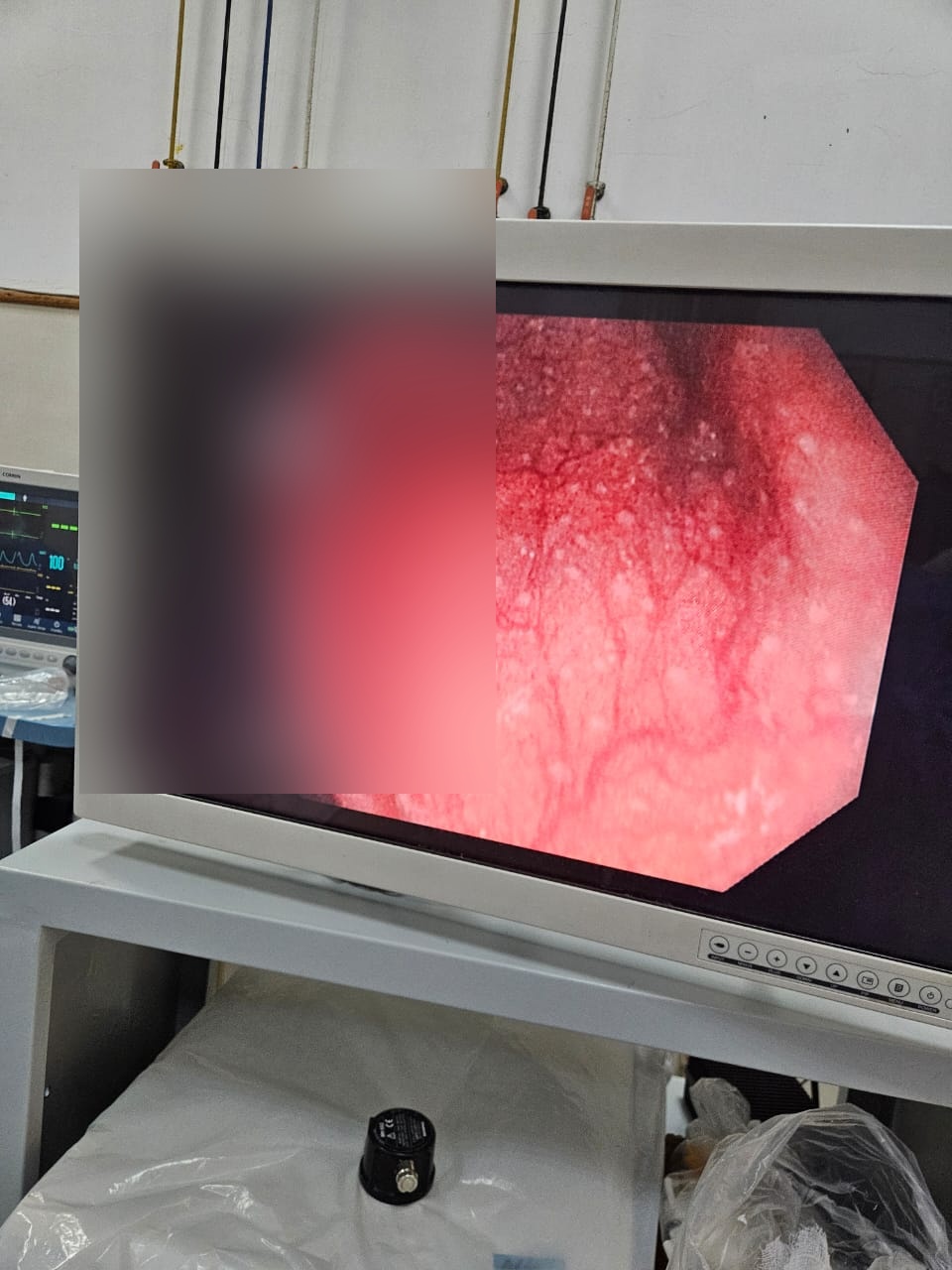
Whitish spots in the colon of a 75-year-old were identified as benign lymphoid hyperplasia. These show well on NBI, are most commonly found in the cecum, and can have a vanilla-brown color. Not to be confused with melanosis coli.
Got a tough case? Drop it in the WhatsApp group. We are 1,000+ endoscopists strong, learning from each other every day.
Every case in this digest comes from real conversations in the EndoCollab private WhatsApp community, 1,000+ practicing endoscopists discussing cases daily from every continent. Lifetime members get permanent access to the group, plus the full EndoCollab case library of 1,700+ teaching cases, technique videos, and references.


