Case Report
An 80-year-old patient on immune checkpoint inhibitor therapy presented with acute right lower abdominal pain mimicking appendicitis. CT revealed free air below the liver, and laparotomy confirmed a perforated duodenal ulcer — a rare presentation known as Rodolfo Valentino Syndrome.
Joel Joseph, MD
Department of Gastroenterology, Carilion Memorial Hospital, Virginia Tech Carilion School of Medicine, Roanoke, USA
Dr. Joseph is a gastroenterologist at Virginia Tech Carilion School of Medicine with clinical expertise in diagnostic and therapeutic endoscopy and complex gastrointestinal conditions.
Klaus Mönkemüller, MD, PhD, FASGE, FJGES, FESGE
Department of Gastroenterology, Carilion Memorial Hospital, Virginia Tech Carilion School of Medicine, Roanoke, USA
Dr. Mönkemüller is a Professor of Medicine and internationally recognized expert in advanced endoscopy. He has published over 400 peer-reviewed articles and is a Fellow of the American Society for Gastrointestinal Endoscopy (FASGE), the Japanese Gastroenterological Endoscopy Society (FJGES), and the European Society of Gastrointestinal Endoscopy (FESGE).
Published: December 27, 2025
Abstract
Background: Valentino’s syndrome is a rare condition caused by irritation of the peritoneum due to fluid from a perforated duodenal ulcer migrating into the paracolic sulcus, mimicking acute appendicitis or other causes of right lower quadrant pain.
Case Presentation: An 80-year-old patient with lung cancer on immune checkpoint inhibitor therapy presented with acute right lower abdominal pain, elevated inflammatory markers, and mild lactic acidosis. CT showed free air below the liver. During laparotomy, a perforated duodenal ulcer was found with a sealed perforation, inflammatory adhesions, pus in the infrahepatic space and right paracolic gutter, and necrotic omentum adjacent to an abscess cavity.
Conclusion: Inserting a fully sealed omentum around the perforated duodenal ulcer led to a presentation indistinguishable from acute appendicitis. Awareness of Valentino’s syndrome is critical to avoid misdiagnosis and unnecessary appendectomy.
Keywords: Valentino’s syndrome; perforated duodenal ulcer; appendicitis; right lower quadrant pain; peptic ulcer perforation; immune checkpoint inhibitor
★ Key Clinical Takeaways
- Valentino’s syndrome occurs when fluid from a perforated duodenal ulcer tracks along the right paracolic gutter and irritates the peritoneum at the right iliac fossa — producing a clinical picture indistinguishable from acute appendicitis.
- Free air on CT below the liver (subhepatic pneumoperitoneum) should raise suspicion for duodenal perforation, even when the presentation clinically resembles appendicitis.
- Immune checkpoint inhibitor therapy can precipitate GI ulceration and perforation — this complication should be considered in oncology patients presenting with acute abdomen.
- The classic teaching of right lower quadrant pain + free air = perforated appendix may be misleading; a perforated peptic ulcer must always be in the differential.
- Prompt surgical exploration is essential; omental patch repair is the standard treatment for sealed duodenal perforations.
Introduction
Valentino’s syndrome — named after the silent film star Rodolfo Valentino, who died in 1926 following a perforated duodenal ulcer initially misdiagnosed as appendicitis — describes the clinical scenario in which fluid leaking from a perforated duodenal ulcer migrates through the right paracolic gutter to the right iliac fossa, producing peritoneal irritation that closely mimics acute appendicitis (1).
The syndrome is a rare but clinically important masquerade. Misdiagnosis can lead to unnecessary appendectomy and delayed definitive treatment of the underlying perforation. With the increasing use of immune checkpoint inhibitors (ICIs) in oncology, clinicians should be aware that ICI-associated GI toxicity — including ulceration and perforation — can precipitate this presentation in a new population of patients (2).
We report a case of Valentino’s syndrome in an elderly patient with lung cancer on pembrolizumab, highlighting the importance of maintaining a broad differential when evaluating right lower quadrant pain in this setting.
Case Presentation
An 80-year-old patient with lung cancer on immune checkpoint inhibitor (pembrolizumab) therapy presented to the emergency department with acute onset right lower abdominal pain, fever, and elevated inflammatory markers. The clinical picture was highly suggestive of acute appendicitis. Laboratory values revealed leukocytosis and mild lactic acidosis.
CT of the abdomen and pelvis demonstrated free air below the liver in the subhepatic space (Figure 1) and inflammatory changes extending along the right paracolic gutter toward the right iliac fossa — a finding consistent with Valentino’s syndrome from a proximal GI perforation.
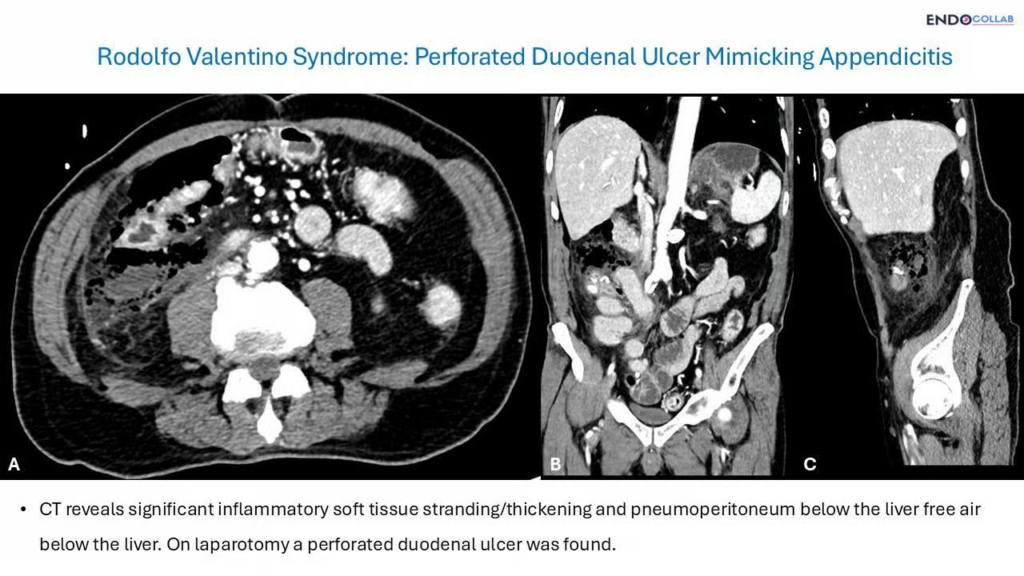
The patient was taken to the operating room for emergency exploratory laparotomy. Intraoperative findings included a sealed perforated duodenal ulcer (anterior bulb) with omental adhesions, purulent fluid in the infrahepatic space and right paracolic gutter, and a necrotic omental patch adjacent to an abscess cavity. The appendix appeared normal. An omental patch repair of the duodenal perforation was performed with peritoneal washout.
Postoperatively, pembrolizumab was discontinued given the suspected ICI-related gastrointestinal toxicity contributing to ulceration. The patient recovered well and was discharged on a proton pump inhibitor regimen with outpatient gastroenterology follow-up.
Discussion
Valentino’s syndrome remains an uncommon but important diagnostic pitfall. The anatomic basis lies in the embryologic continuity between the right paracolic gutter and the right iliac fossa: fluid from a duodenal perforation can freely track inferiorly, irritating the parietal peritoneum at McBurney’s point and producing rebound tenderness, guarding, and pain that is clinically indistinguishable from appendicitis (1).
The presence of free air on CT — particularly in the subhepatic space — should always prompt consideration of a proximal GI source, even when the clinical presentation favors appendicitis. In this case, the combination of subhepatic pneumoperitoneum and right paracolic inflammatory changes was the key imaging clue (3).
The increasing use of immune checkpoint inhibitors in cancer treatment has introduced a new population at risk for GI perforation. ICIs can cause immune-mediated gastritis, duodenitis, and ulceration — even in patients without prior ulcer history (2). Clinicians managing oncology patients on ICIs should maintain a high index of suspicion for this complication when patients present with acute abdominal pain.
This case reinforces the classical lesson: the combination of right lower quadrant pain and pneumoperitoneum does not always mean a perforated appendix. Valentino’s syndrome should be part of every surgeon’s and gastroenterologist’s differential diagnosis in such presentations.
Conflict of Interest
No conflicts of interest declared by JJ or KM with any of the companies, devices, or products mentioned in this article.
How to Cite
Joseph J, Mönkemüller K. Rodolfo Valentino Syndrome: Perforated Duodenal Ulcer Mimicking Appendicitis. EndoCollab. December 27, 2025. Available at: https://endocollab.com/blogs/gi-endoscopy-tips-tricks/rodolfo-valentino-syndrome-perforated-duodenal-ulcer-mimicking-appendicitis/
References
- Vakili K, Pomfret EA. Biliary anatomy and embryology. Surg Clin North Am. 2008;88(6):1159-1174. [Valentino’s original presentation context — classic reference on paracolic sulcus anatomy and right lower quadrant peritonitis from proximal GI sources.]
- Marthey L, Mateus C, Mussini C, et al. Cancer immunotherapy with anti-CTLA-4 monoclonal antibodies induces an inflammatory bowel disease. J Crohns Colitis. 2016;10(4):395-401.
- Mönkemüller K, Fry LC, Eloubeidi M. Perforated Duodenal Ulcer Presenting as Appendicitis: Valentino’s Syndrome. Endoscopy. 2009.

