CASE REPORT
Authors:
Juan De Dios Díaz Rosales, MD, MSc
Gastrointestinal Endoscopy Surgeon at Instituto Mexicano del Seguro Social and Universidad Autónoma de Ciudad Juárez. His clinical and academic interests include digestive diseases, biliary tract disorders, and therapeutic endoscopy.
Daniel A. Portillo-Rodríguez, MD
PGY-2 Resident, Hospital General de Zona No. 35. Dr. Portillo-Rodríguez is an early-career researcher and earned his medical degree from the Universidad Autónoma de Ciudad Juárez.
Clinical History
A 61-year-old woman presented with two weeks of postprandial upper abdominal pain, mild scleral icterus, dark urine, and a palpable right upper quadrant mass. Laboratory tests showed a mixed hepatocellular-cholestatic pattern: total bilirubin 2.31 mg/dL, direct bilirubin 1.77 mg/dL, AST 259 U/L, ALT 290 U/L, alkaline phosphatase 231 U/L, and GGT 852 U/L. Abdominal ultrasound demonstrated a markedly distended gallbladder measuring 138 × 63 × 55 mm, with sludge and multiple stones, the largest measuring 25 mm, without intrahepatic bile duct dilation. Non-contrast CT confirmed gallbladder hydrops and cholelithiasis, with a gallbladder measuring approximately 120 × 66 × 69 mm and heterogeneous intraluminal content.
ERCP Findings and Intervention
ERCP was performed because the biochemical profile and mild jaundice suggested functional biliary obstruction despite the absence of significant bile duct dilation on initial CT imaging. The initial cholangiogram demonstrated opacification of the extrahepatic bile duct with a smooth extrinsic indentation and focal narrowing of the proximal-to-mid common bile duct, without an obvious intraductal filling defect. The was proximal dilation of the bile ducts. This configuration was considered compatible with pseudo-Mirizzi syndrome in the setting of a markedly distended gallbladder filled with stones (Figure 1). After biliary sphincterotomy, balloon sweeping was performed. The post-sweep cholangiogram showed improved ductal clearance, preserved distal bile duct patency, and no definite residual filling defects, supporting the absence of retained choledocholithiasis after endoscopic extraction maneuvers (Figure 2). Given the extrinsic inflammatory deformation of the bile duct and the anticipated high-risk surgical anatomy, a plastic transpapillary biliary stent was placed to secure internal drainage and maintain ductal decompression (Figure 3).
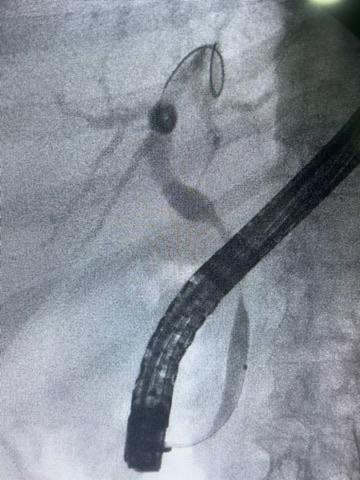
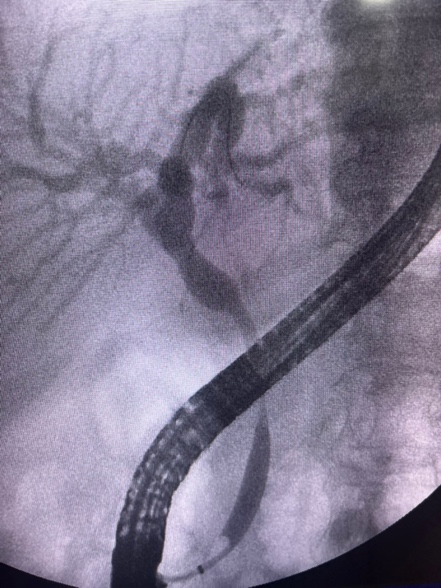
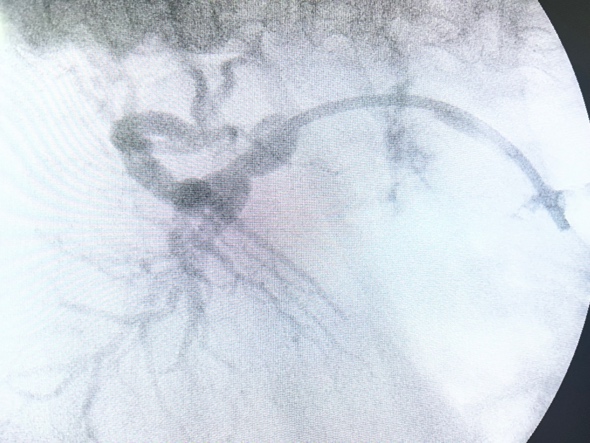
Teaching Point
Subsequent surgery confirmed an obliterated hepatocystic triangle, consistent with vanishing Calot anatomy. The key teaching point is that pseudo-Mirizzi on ERCP should alert both the endoscopist and the surgeon that the problem is not merely intraductal. Extrinsic biliary compression from a hostile gallbladder neck or infundibular inflammatory process may be the fluoroscopic signature of a dangerous Calot dissection. In this setting, endoscopic biliary drainage can serve as a bridge to safer surgical management, and the operative strategy should prioritize avoidance of major bile duct injury over completion of a conventional cholecystectomy.
References
Mercado MA, Rueda De Leon A, Cisneros-Correa J. Vanishing Calot Syndrome: Pseudo-Mirizzi Syndrome. J Am Coll Surg. 2020;230(5):841-842. doi: 10.1016/j.jamcollsurg.2020.01.036.
Mergener K, Enns R, Eubanks WS, Baillie J, Branch MS. Pseudo-Mirizzi syndrome in acute cholecystitis. Am J Gastroenterol. 1998;93(12):2605-2606. doi: 10.1111/j.1572-0241.1998.00559.x.
Brunt LM, Deziel DJ, Telem DA, et al. Safe Cholecystectomy Multi-society Practice Guideline and State-of-the-Art Consensus Conference on Prevention of Bile Duct Injury During Cholecystectomy. Ann Surg. 2020;272(1):3-23. doi: 10.1097/SLA.0000000000003791.

